Journey to the Chemo Ward
Thank you, THANK YOU to my friends and family who have poured out love and prayer and healing energy to me. Please know, even if you don’t receive a personal response from me right now, I see you and feel your love. I hope providing these wider updates helps keep those interested in the loop.
January 2026, for me, started under an umbrella of feeling ‘generally shitty’. Starting with a gnarly respiratory cold and ending with stomach flu. Nothing too out of the ordinary, as I often get sick around the holidays. In early February, I noticed shortness of breath when hiking up the three flights of stairs to my apartment. Surprising, since only months before I moved a 75 lb bed up those stairs. In mid-February, I had the opportunity to jet off to the Joshua Tree desert with some sober girlies. I barely made it a few huffs on the Ryan’s Mountain path when I felt like I couldn’t pull in any air and my chest played hard-rock palpitations in my ears, and the edges of the cactuses glinted with white stars.
I perched on a rock, looking out over the vastness, and felt distinctly “you’re ok AND something is not right”. Thankfully, I already had an appointment with my primary care doctor scheduled for late March.
Deserts make me feel things. Desserts, too.
Two weeks before my originally scheduled appointment, it was a Friday afternoon, and I was talking to my co-worker. Halfway through a sentence, I couldn’t gather enough breath to speak, and that, my friends, is when I really got scared. I love to talk. I went home that weekend, and my body essentially said: “Enough is enough, bish, listen to me, we are not ok”. I couldn’t stand for more than 10 minutes without feeling short of breath and nauseous. Lying down felt worse. I moved up my appointment to that Monday, Monday, 3/17, and that’s when the real show started.
Let me preface real quick that I’m sharing my experience in a tone of voice that feels comfortable for me. Sometimes staunchly honest, often silly…but please know I in no way take this or anyone else's health diagnosis lightly. We heal with the medicine that serves our personality. Take what you need from me; however, know that your experience or that of your loved ones has all the space to be shared and felt in a way that is true to you and/or them.
Call it a blur, a whirlwind, a catatonic boom followed by chaos: a visit to my primary care doctor quickly escalated to a chest exam to a CT exam to an appointment with a pulmonologist and then admission to the 14th floor of the hospital. I mean this genuinely, my 36 years have been deeply blessed with few doctor's visits and no hospital visits. I was the new girl on the block, and my blood pressure and heart rate were showing off (not in a good way).
I met with an oncologist. Things were serious. They’d discovered a 17 cm mass in my pericardial area. The formal title of the cancer presented: Primary mediastinal large B-cell lymphoma (PMBCL). And she came with a lot of fluid that was growing unstable around my heart. It was time for a group of doctors to make some serious plans.
What hit me the most: the impact the chemo would have on my chances of fertility. In one beat, I felt relieved when my doctor referred to my age as the “height of childbearing years”. Especially since my period app and every other outdated internet source consider 36 geriatric in terms of pregnancy. In the next beat, I was on my hands and knees, crying because I felt a tear within me. As someone who believes the female body goes beyond producing…I’ve always found the concept magical. And only previously that year had I granted myself permission to believe I was capable and worthy of carrying a child. The doctor went through some options for freezing my eggs. All of which would involve more severe treatment happening at the same time as chemotherapy treatment. I listened to what my body and heart wanted. They wanted the chance to survive, with the faith that a family isn’t defined solely by genes. I felt relief when I decided that it was my body and my chemo treatment that would take full priority. I’ve always lived in a queerer reality of parenthood. Knowing I want to care for someone, and also knowing they may not come from my body or genes. I felt relieved when I made my decision.
Spying on Fred & George. When I was delayed in the CCU the hardest feeling, pure emotion and sans logic, was that I would never see them again.
I took up residence for almost a week on the 14th floor while they did PET scans and took a biopsy of The Stranger in my chest. I chewed on French toast from the cafeteria, caught up on Paradise, and laughed A LOT with the family who visited me.
My chemo treatment plan was set, my oncologists were optimistic and ready, and then enter stage right - the cardiologist with concerns. The fluid around my heart was turning into an unrelenting compression sock, and he wanted to drain it before chemo started. They whisked me into surgery to install a draining system and dropped me off in the Critical Care Unit, where the darkest part of my journey thus far started.
We found ourselves in a catch-22. The chemo would eventually help reduce and stop the fluid; however, the cardiologist wanted to be sure that enough fluid had been safely removed before starting chemo. I was visited by too many doctors and nurses at this time to even begin to track them. All saying the same thing: “emoji of guy shrugging his hands”. The Critical Care Unit is not a hospitable place. It’s where the severely ill are treated. Although I felt grateful to be relatively well in comparison…I felt misplaced and forgotten. Except for every six hours when someone took a syringe to my chest to painfully extract fluid. It felt like someone tugging out a vein, over-twisted like a long chord, and that chord was being pulled from somewhere, also in my shoulder blade and also around my teeth.
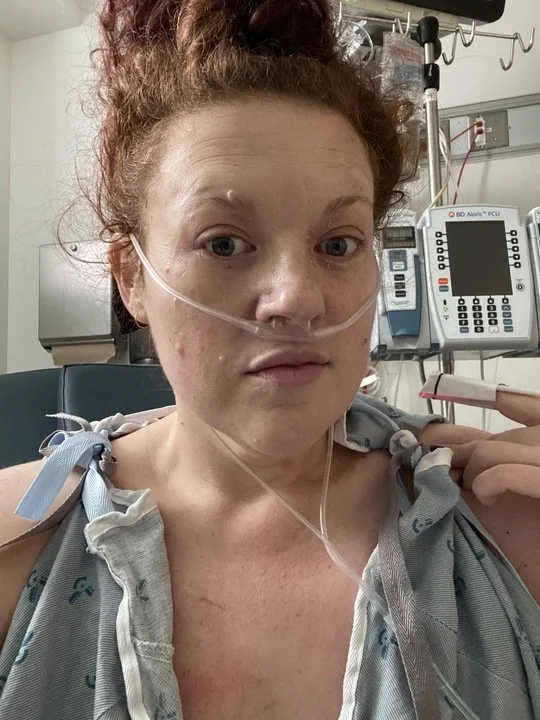
The face of a girl who wants NO unsolicited doctor backrubs, please. Just updates.
A second surgery was planned. They were going to implant a pericardial window in the cavity surrounding my heart so fluid could continue to drain while I begin my chemo treatment. The plan was to open up that window and move me to the 20th floor (the chemo ward) immediately.
First, the surgery was delayed a day. Then, post-surgery, they returned me to the CCU. Then, I, the positive star child of the hospital, crumbled like a house of soggy graham crackers. The anxiety meds couldn’t touch my panic. It felt like I would never leave the windowless CCU. After every day, building myself up for the eventual chemo treatment only to be told that it is happening ‘later - can’t give you a date - but later’, I felt the bottom of a dry reserve of hope. And the pain, unlike anything my body had yet to endure, challenged my newly given identity as ‘a warrior’. That really scared me. I called my mom and aunt at this point - having nothing left to argue and understandably not really believing the blur of faces telling me “something would change sometime soon”.
After over a week without touching grass or seeing the outside and after over a week without a shower…the slow IV-like drip of humanity began catching speed and the color leaked from the four walls around me.
I didn’t want to see anyone except my oncologist, and I didn’t want to hear anything except ‘we are moving you, at last, to the 20th floor’.
My nurse at the time, Meagan (great name), championed this moment. Also getting annoyed with the ambiguity. First, she was like, “Get this girl her oncologist and stat!” Then she called the 20th-floor supervisor and learned I was a special admit. They (oncology) had been anxiously awaiting me for a week and were also a bit flummoxed by the delay from cardiology. No shade to cardiology - but they were clearly operating in their lane with blinders on - probably for good reason, and I felt valid frustration. Within an hour, Meagan personally delivered me to the 20th floor, and later that evening, I started my first round of chemo. I have been here ever since and will be discharged from the first cycle on Friday, 4/3.
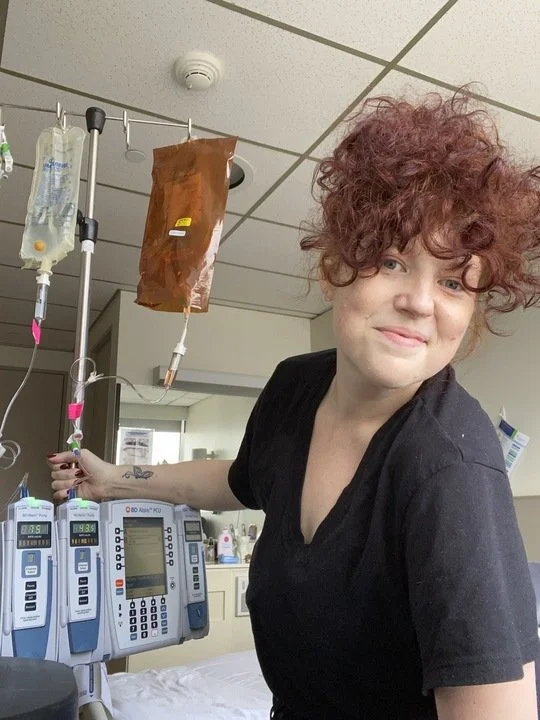
Unlike in the CCU, I’m only hooked up to two things (both of which allow mobility). Chemothina - my dancing and walking partner who is pumpin’ out cancer-killin juice 24 hours straight for the first 4 days. Plus BeatBoxBuddy, this heart monitor that fits in my pocket and lets the nurses know that my resting heart rate is taking a less manic approach to existing.
For those interested in the Google search of it all: my chemo plan is R-EPOCH. I do 5 days of inpatient treatment, and then I go home for ~ 2 weeks to recover (and co-exist in the presence of my cats, Fred and George), and then I return for my next cycle. I will complete 6 cycles in total. My treatment plan lasts until ~ the end of July.
Oh hey, do I spy some light behind those bebe blue eyes?
I will lose my hair. I will feel nauseous and unwell and sleepy and and and…we will discover as we embrace it moment by moment.
My reservoir of hope is already refilled. I’m so lucky to be in a room with a view of the Houston cityscape. I receive visitors every day, and believe it or not, I have managed to sleep.
I’ve discovered that The Veggie from Jersey Mike’s is my favorite post-surgery fast feast. I’m humbled to learn you can be 36 and still shit your joggers. My belly is a constellation of bruises from the blood thinners. I do my laps around the ward humming the ‘Mishberach” and practicing tonglen. I’m changing, and it’s not just because I have cancer. It’s because of how I’m choosing to face down cancer. I have a lot of goals, pockets full of hope, and a village of humans and cats rallying at my side.
Until we speak again, I love you -
Sincerely, Nutmeg